New Brunswick is Moving Cervical Cancer Screening Home
With $5 million for at‑home screening in the 2026-27 budget, the province joins a national push to eliminate a disease that hits rural and low‑income communities hardest
Stay in the Know.
If this story piqued your interest, please share it. Every share helps spread knowledge about the ins and outs of local affairs and keeps independent reporting strong on Canada’s East Coast.
There is no joy in a woman’s heart when she hears her doctor say, ‘scooch down.’
Naked from the waist down, covered by a hospital-grade sheet, with her feet in bootie-covered metal stirrups, she wiggles across the paper-lined table to its edge, lies down and braces herself.
That’s how the pap test begins. It ends with her doctor taking a swab of her cervix, so its cells can be tested.
So it is for trans, non-binary and Two-Spirited people too.
It’s an uncomfortable test for a horrible disease: cervical cancer.
The 2026-27 New Brunswick provincial budget, tabled on March 17, commits $5 million to expand cancer screening programs – including making at-home cervical screening available to New Brunswickers for the first time.
It would make New Brunswick the second province in Canada, behind British Columbia, to provide at-home cervical cancer screening.
The Numbers
An estimated 1,600 people in Canada were diagnosed with cervical cancer in 2024 and about 400 died from it, according to the Canadian Partnership Against Cancer, a federally funded non-profit that facilitates a pan-Canadian approach to cancer control.
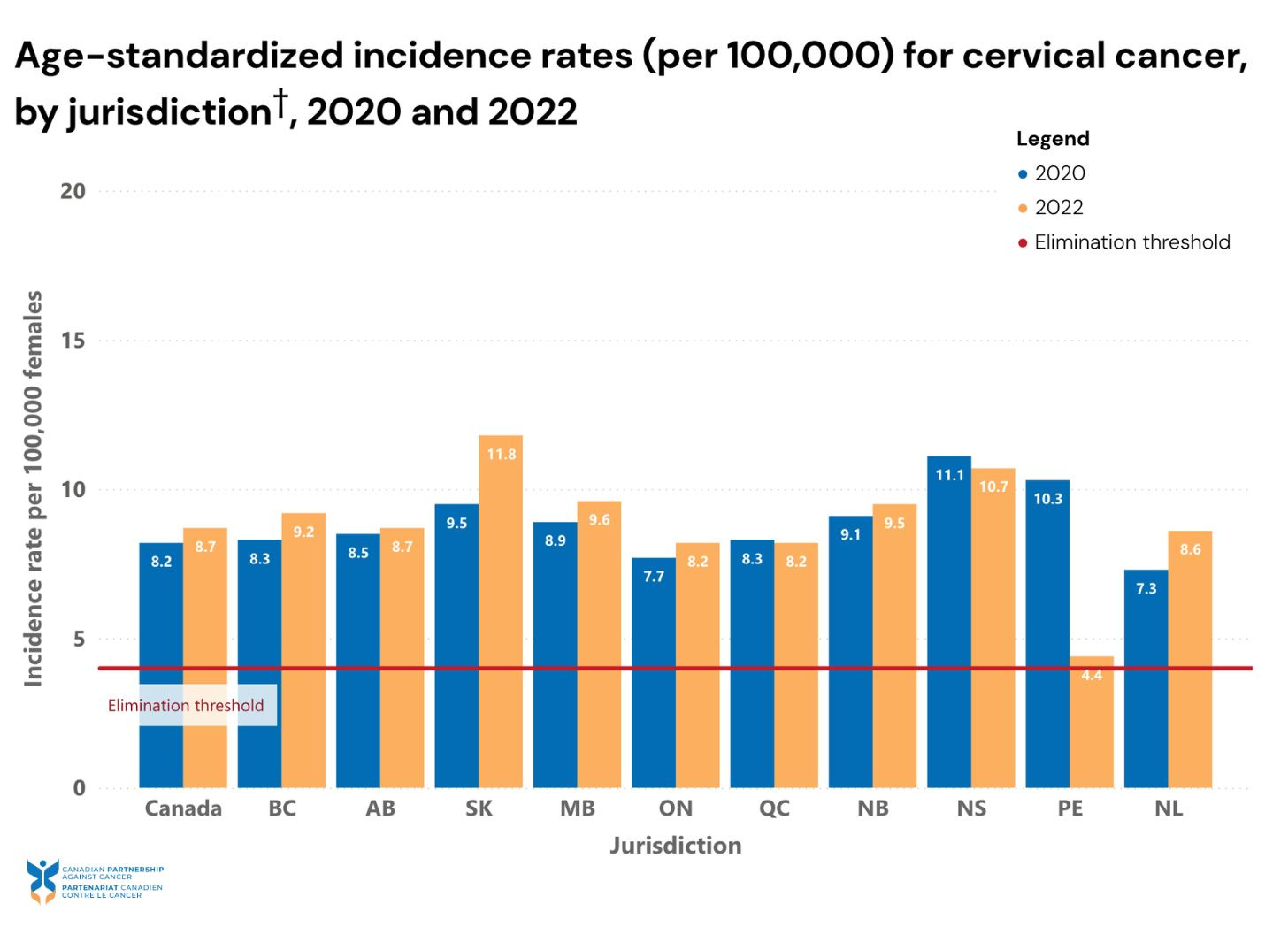
There were 8.7 cervical cancer cases per 100,000 females in Canada in 2022, more than double the threshold of four per 100,000 that the World Health Organization (WHO) defines as required to eliminate the disease.
New Brunswick’s numbers sit at around 9.5 cases per 100,000. Nova Scotia sits at 10.7, Newfoundland and Labrador at 8.6, and PEI at 4.4 cases per 100,000 – the lowest in the country.
Cervical cancer incidence rates are higher among people in lower-income neighbourhoods and rural areas – the group of people that home-based screening is designed to reach.
It doesn’t have to be like this because cervical cancer can be eliminated through vaccinations, which New Brunswick has offered in schools since 2008, and is highly treatable when detected early.
Hence, the two-step public health policy approach to cervical cancer in Canada: increase vaccination rates to try to eliminate cervical cancer by 2040, and increase testing and early detection to treat it.
Beyond The Doctor’s Office
This is where the traditional Pap test at the doctor’s office falls short.
Getting to a clinic, booking time off work, arranging childcare, and then enduring the physical discomfort of a speculum exam are collectively significant deterrents. For survivors of sexual trauma, it can be much worse, and for people without a regular family doctor, it can be effectively impossible.
The at-home alternative works differently. Instead of a clinician collecting cells directly from the cervix, the test uses a small swab to take a sample from the vagina to look for human papillomavirus (HPV), the virus that causes cervical cancer.
A person collects the sample by turning the small swab inside their vagina for 20 seconds; the sample collected is just as accurate as a provider-taken sample. The completed kit is mailed back in a prepaid envelope, much like New Brunswick’s at-home colon screening tests.
British Columbia became the first province to offer at-home testing province-wide in January 2024. In its program, a clean HPV result means no further screening is needed for five years, compared to every three years with a Pap test.
New Brunswick announced its intention to make this transition back in 2023, but the rollout stalled. The $5 million in the 2026-27 budget is designed to get it moving.
Who Should Get It
Anyone with a cervix, including women and Two-Spirit, transgender and non-binary people, between the ages of 25 and 69, should screen for cervical cancer, whether or not they’ve had the HPV vaccine, whether or not they’re currently sexually active, and whether or not they’ve been through menopause.
People who are pregnant, or experiencing symptoms like bleeding between periods or unexplained pelvic pain, should still see a health-care provider rather than relying on self-screening.
HPV primary screening with timely and appropriate follow-up has been implemented or partially implemented in Prince Edward Island, British Columbia, Ontario, Québec, and the Northwest Territories, and is being actively planned in the other provinces.
Canada has committed to eliminating cervical cancer by 2040. Reaching that target requires 90 per cent of eligible people to be screened with an HPV test by 2030. Cervical cancer rates are especially high among people in rural or remote areas, people with low incomes, and likely, though data is limited, among 2SLGBTQIA+ individuals and people who identify as Indigenous or Black, due to structural and systemic barriers in the health system.
For those groups, a home kit that arrives in a plain envelope and can be completed in private may be the difference between screening and not screening at all.
Support Local Storytelling & Reporting
Want more analysis like this? Becoming a paying supporter of Side Walks and follow our continuing coverage of the issues shaping Atlantic Canada’s future.
Stroll Over to Side Walks For More Stories
AI-enabled summary: New Brunswick’s latest budget commits $5 million to at‑home cervical cancer screening, expanding HPV testing and removing barriers faced by rural and low‑income communities. The move aligns New Brunswick with a national push to eliminate cervical cancer by 2040 through improved early detection and prevention.
Keywords: New Brunswick cervical cancer screening, at‑home cervical cancer test, HPV testing Canada, Pap test alternative, New Brunswick health budget, cancer screening programs Canada, cervical cancer prevention, rural health care access, HPV primary screening, eliminate cervical cancer Canada.





